Australian IVF Breakthrough: Stick-On Patch Could Replace Blood Tests
Researchers have unveiled a revolutionary stick-on patch that could transform the IVF experience for thousands of Australian women, replacing constant blood tests and potentially increasing the chances of successful pregnancy. This innovative device, developed by researchers at Monash IVF and the University of Melbourne, would allow patients to monitor their hormone levels at home, eliminating the need for multiple blood tests during each IVF cycle.
Current IVF Process Described as Gruelling
For women undergoing IVF, the current process is gruelling. Luciana Charry, who has undergone multiple cycles, described her experience: “I’ve been through about three cycles of IVF, five embryo transfers.” She highlighted the challenges: “Blood tests, the scans, the needles, the injections.” Currently, doctors rely on blood work to pinpoint the optimal windows for collecting eggs and embryo transfers, forcing patients to undergo multiple tests every round.
Associate Professor Mark Green from Monash IVF explained: “In a normal cycle there’s probably anywhere between three to five blood samples that they’d have to have taken in that cycle.” The new biosensor patch aims to reduce this burden significantly.
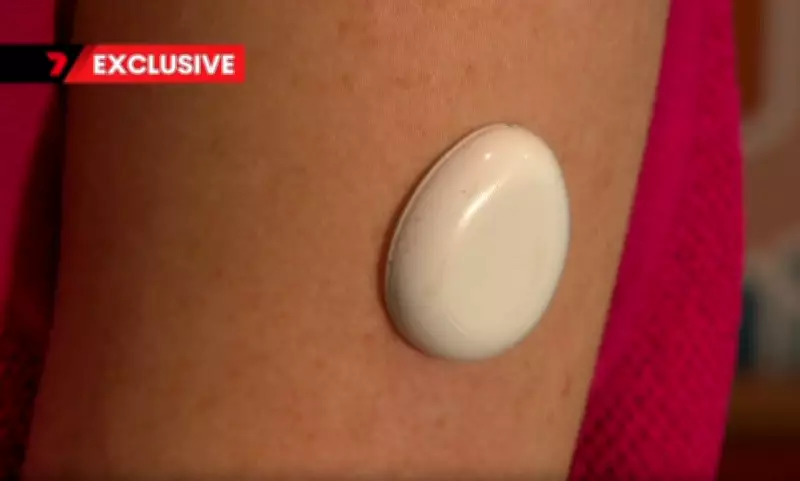
How the Biosensor Patch Works
The new biosensor patch uses tiny microneedles to measure progesterone and oestradiol levels, key hormones in IVF treatment. “These are very tiny microneedles that we’re using, and so there’s less pain involved,” Green said. This technology offers a major convenience factor as it is accessible from home, allowing patients to avoid frequent clinic visits.
Once the device reads the hormones, patients can Wi-Fi the results directly to their doctor and nurse for clinical decisions. “That hopefully will lead to better chances of success for that pregnancy,” Green added, emphasising the potential benefits for treatment outcomes.
Future Development and Patient Hopes
While prototypes have been developed, the device is still being fine-tuned before clinical trials begin. Researchers are hoping to roll it out within the next few years, pending further testing and approvals. Luciana Charry expressed optimism: “I believe it’s going to make a huge difference,” reflecting the hope among many IVF patients for less invasive and more effective treatment options.
This breakthrough represents a significant step forward in reproductive health technology, aiming to make IVF more accessible, less stressful, and potentially more successful for women across Australia and beyond.









